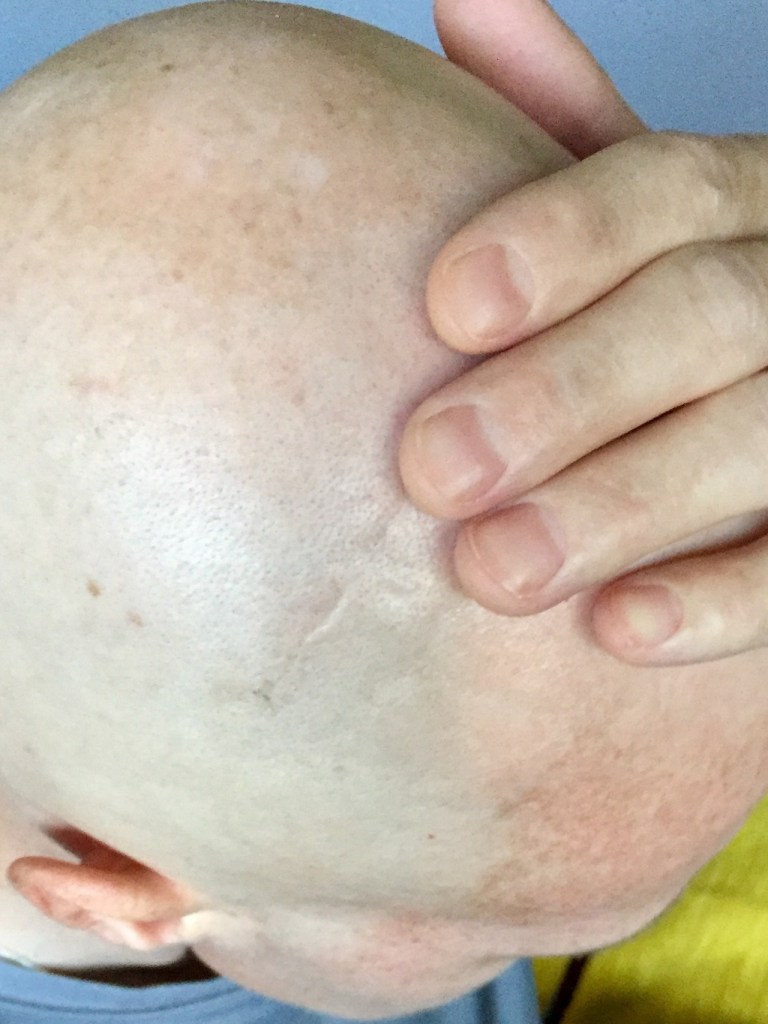
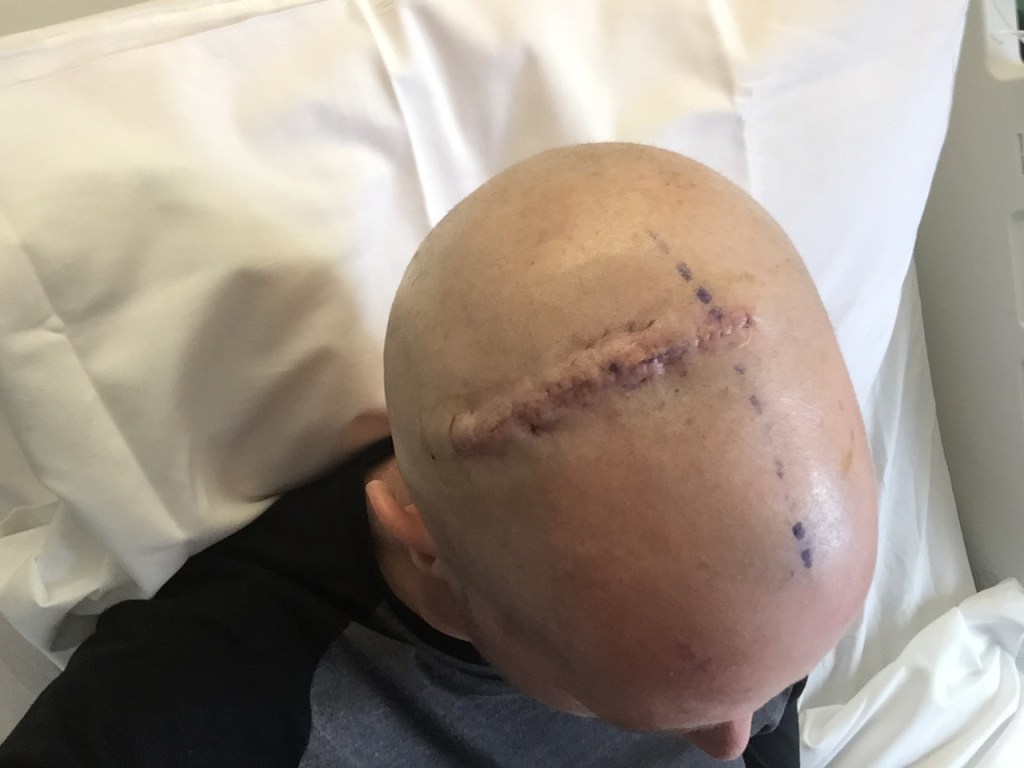
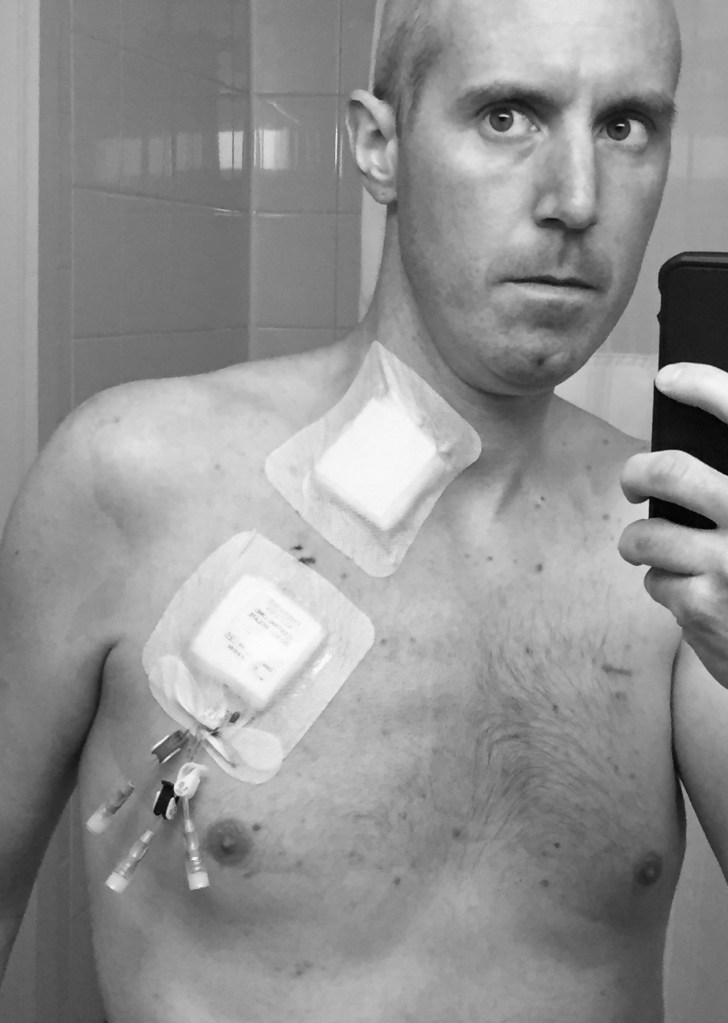
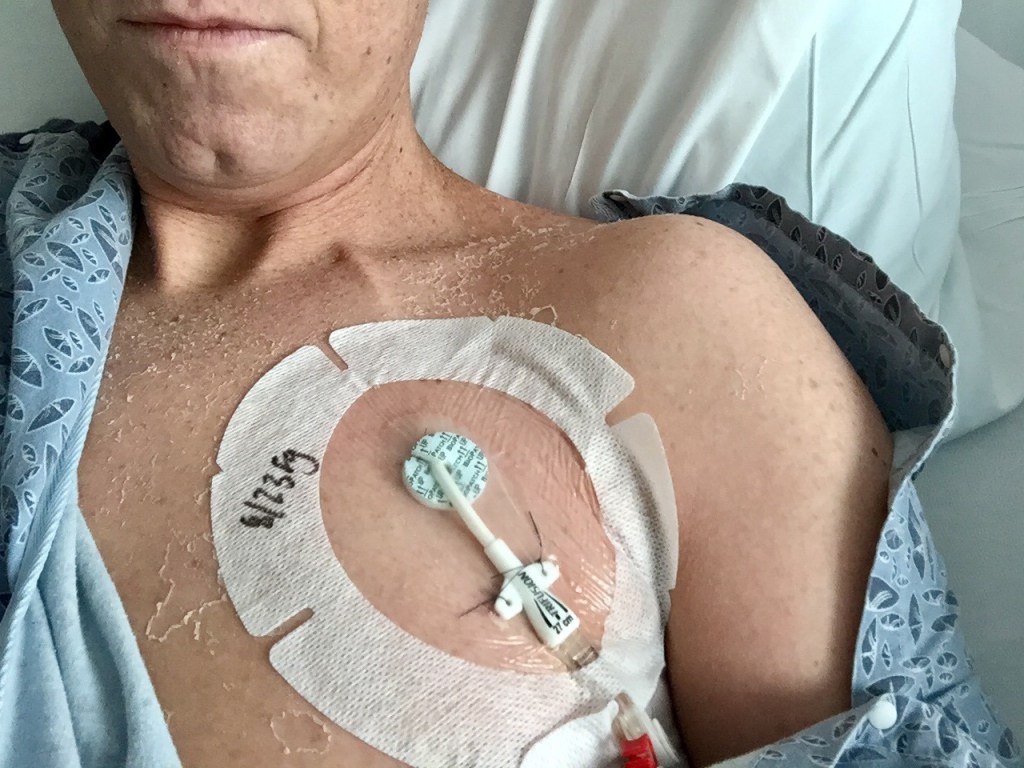
I have witnessed my hair fall out three different times due to chemotherapy treatment. The first time was quite a shock. I looked down one morning to see hair covering my pillowcase. But the real shock came when realizing how quickly it happened, how quickly the chemicals flooded my system and started killing off cells. My very first “conventional” round of chemo was administered on a bi-weekly basis, if I remember correctly. This gave me a week in between to rest and recover before the next round. Because the timing of everything was so fast, I started the first round of treatment almost immediately after returning home to New England and, as such, had a full head of hair and a beard. Some people cut their hair close and shave preemptively before treatment, but I didn’t have time. Anyway, on the first off-week, the first week between cycles, I awoke one morning and discovered my pillowcase covered in my hair. That same morning, I stood in the shower and watched as the water deepened due to the clumps of hair forming in and around the drain. i didn’t know then that i would witness this shedding (a term i’ve come to enjoy & one i find apt) another two times very shortly.
The sensation of losing one’s hair, especially at the rate at which it falls out due to chemo, is unnerving, to say the least. Hair has always held this sacred energy; it connects to the past and holds information about various aspects of our lives. During treatment, when it begins to fall out in fistfuls, it’s hard to rationalize this loss by saying, “It’s the chemo doing its job,” when one understands it to be the result of the indiscriminate killing off of cells. It doesn’t necessarily target rogue cells or cells that have gone haywire and/or rapidly dividing cells. This has always been the thing that has frightened me about chemotherapy treatment — it is simultaneously saving someone and killing them.
A closely cropped head of (already thinning) hair is the norm for me. However, when the eyelashes fall out and the eyebrows thin to near nonexistence, it is hard to look in the mirror and not feel alien within one’s body.
Just as I’ve witnessed the loss of my hair 3 different times, I’ve also had the pleasure of watching it return. And, in all honesty, it is a pleasurable experience to watch such a seemingly spontaneous rebirth occur. This time around, the timing couldn’t be better. As the days become shorter and cooler, I’m slowly sprouting a new beard & checking daily if the fuzzy growth appears & thickens atop my head.